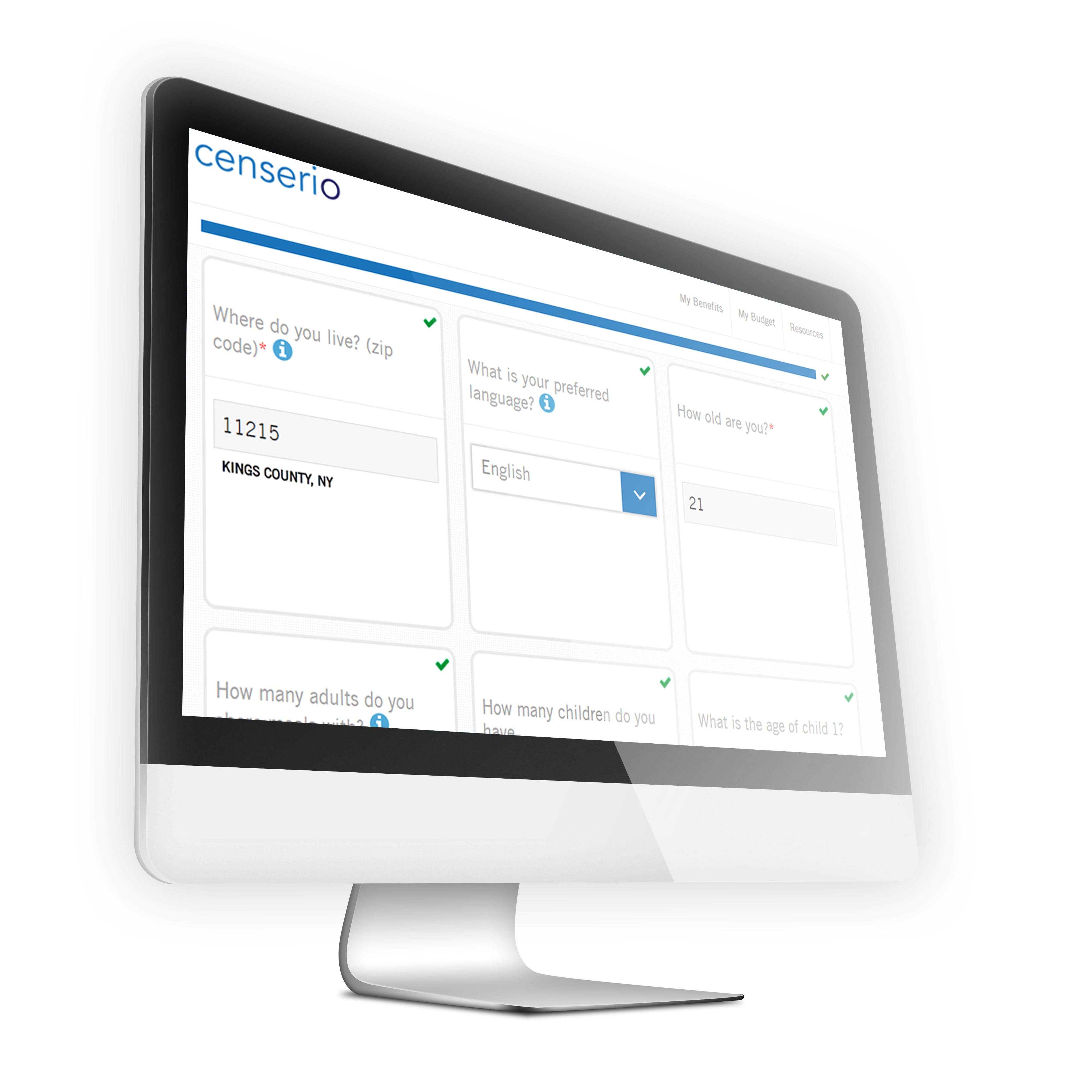
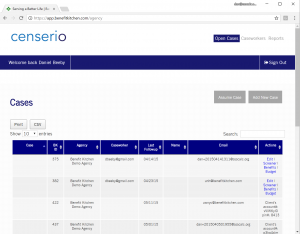
Analytics to create a plan- or provider-specific census
- Track and monitor your high-risk population
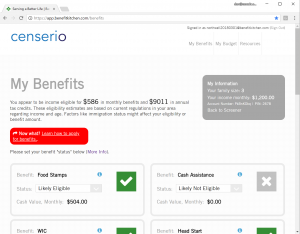
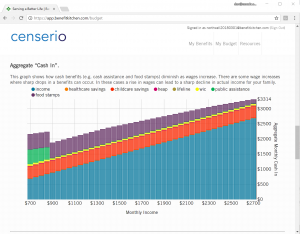
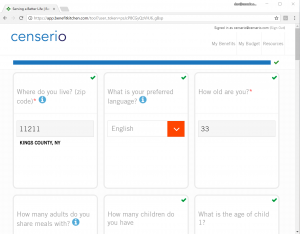
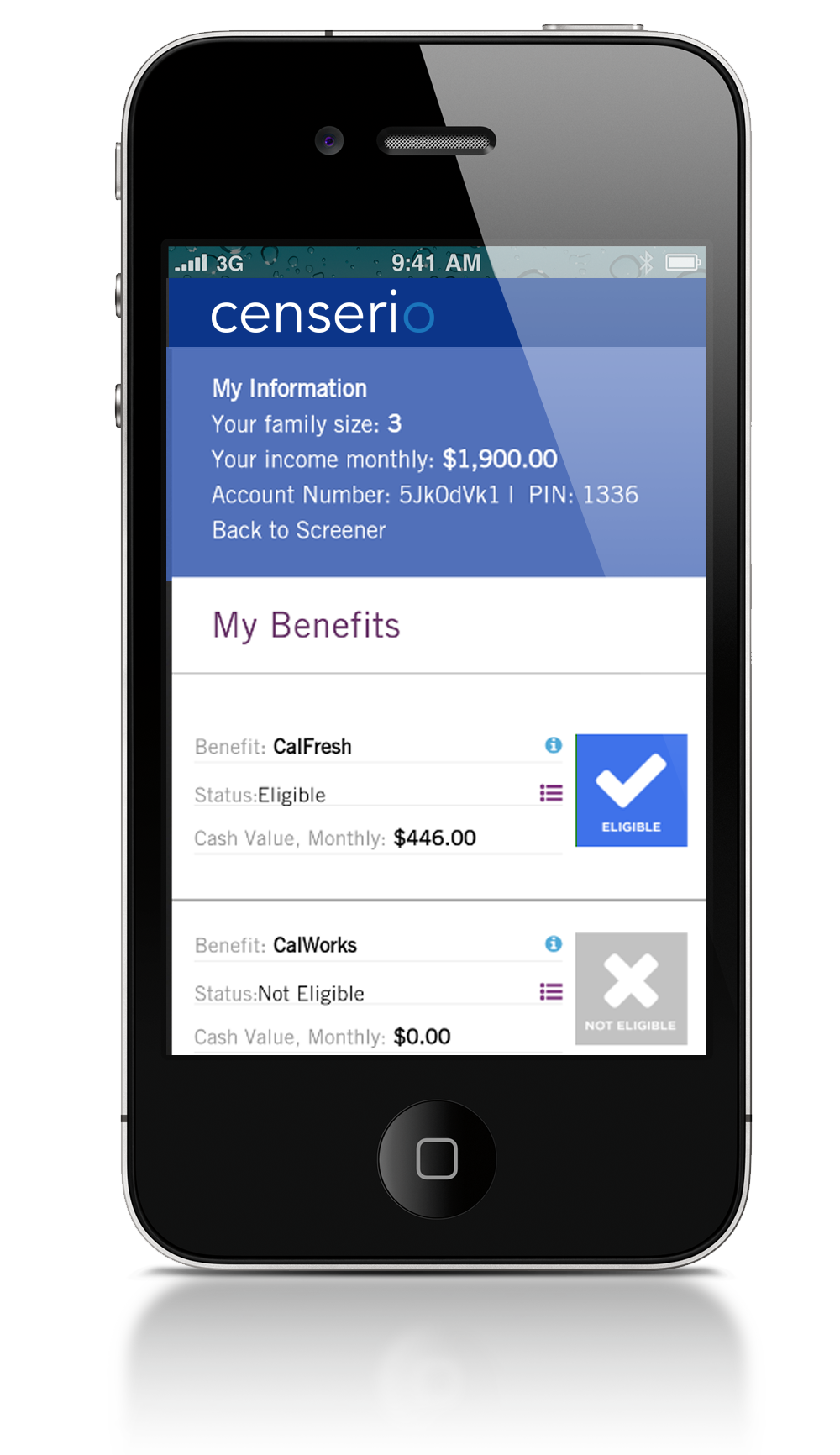
- Identify social benefits and members’ eligibility
- Measure results and quantify program outcomes.
Utilize social programs to control socio-economic health disparities
- Low income does not have to mean high cost
- Offer members housing, food, and childcare security
- Use dashboards to review engagement and outcomes
Lower ED recidivism by promoting household stability
- Connect members with benefits that promote long-term wellness
- Discover to-the-dollar eligibility for up to 18 federal, state and local benefits
- Find local social programs and supports